Medical
Examination
Anorectal examination
Usually a source of acute embarrassment for the prospective patient. One can diffuse that by simple explanation and reassurance. After a brief discussion about relevant health history, both constitutional and specifics relating to the anorectum, the patient is placed in the left lateral Sims position (laying on one’s left side).Visual inspection is the initial step which reveals an abundance of data to the clinician. One must be diligent to observe the perianus, gluteal crease and the perineum. Often times the condition that is responsible for the patient’s symptoms is very apparent. Some of the more common conditions that are usually visible are external hemorrhoids (thrombosed or non-thrombosed), pruritus ani (anal itching), skin tags, HPV (anogenital warts), perianal fistula, sebaceous cyst, Crohn’s disease, anal cancer, anal fissures, etc. The list is very long. Palpation of the surrounding tissue is imperative as tissue density varies with different conditions. Anorectal cancers are indurated masses that will feel like your “forehead”. Hemorrhoids will be more “spongy” like ones chin.

Digital exam
Digital exam is the introduction of the examiners index finger into the anorectum. I apply a 10% Lidocaine (topical) which helps to minimize discomfort. One immediately feels for anal muscle tone or lack thereof. If this is painful, then one must adapt to the patient’s response. If there is significant pain, usually there is an anal fissure, possible anal abscess, anal cancer, etc., and a condition that is very common but under diagnosed, anal stenosis (anal narrowing/anal reflexive spasm). In women I check for rectoceles and in men I may I may palpate their prostate. At the anorectal line one may encounter enlarged hypertrophied anal papilla, which are usually present when one has anal fissure disease. Internal hemorrhoids, as mentioned will feel “spongy” and anorectal cancers will be indurated (hard) and fixed. I always look at my examining finger to check for blood.
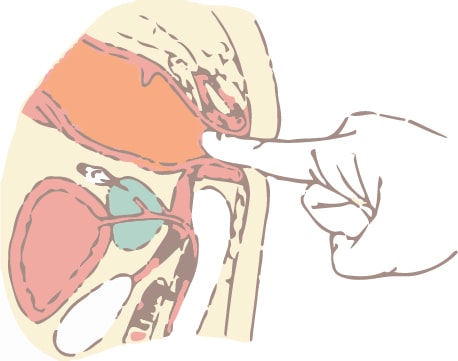
Completion of Exam
We then proceed to examine the anorectum with a Barr-Shuford anoscope.
Adequate lubrication is essential. I inspect for hemorrhoidal disease, anal papilla, rectal polyps, IBS, IBD, Crohn’s disease, etc. and this part of the exam (anoscopy) just takes a few seconds depending upon tolerance and visual findings.
Upon completion, I leave the room and allow the patient to get dressed and we then discuss the findings.